
Food Safety Focus (202nd Issue, May 2023)–Article 2
Sapovirus – Virus causing illness similar to Norovirus
Reported by Dr. Ken CHONG, Scientific Officer,
Risk Assessment Section, Centre for Food Safety
In a recent local food poisoning outbreak involving raw oysters, Sapovirus was detected in the stool samples of an affected consumer and a food handler who had handled the oysters. Sapovirus taxonomically belongs to the same family as Norovirus. Both viruses can cause acute gastroenteritis where clinical symptoms caused by these viruses are indistinguishable. In this article, we will get to know more about sapoviruses in food and relevant preventive measures.
Sapoviruses
Sapoviruses were named after an outbreak of acute infectious diarrhoea that occurred in an infant home in Sapporo, Japan in 1977. Previously the viruses had also been called “Sapporo-like viruses.” Gastroenteritis outbreaks associated with sapoviruses are less common than those caused by noroviruses, both globally and locally. According to a review by the Centre for Health Protection, among 182 outbreaks of acute gastroenteritis voluntarily reported by institutions and schools in 2017, sapoviruses were associated with only 2 outbreaks (1.1%).
Similar to noroviruses, sapoviruses are primarily transmitted by the faecal-oral route and person-to-person contact (e.g. contact with faeces, vomitus or contaminated materials/surfaces) or via contaminated food and drinking water. As such, outbreaks in institutional settings are not uncommon. Although dose-response study for sapoviruses is not available, it is believed that their infectious dose is low, comparable to that of noroviruses.
Gastroenteritis Caused by Sapoviruses
Sapovirus gastroenteritis symptoms are usually self-limiting, and patients usually recover within a couple of days; the symptoms, severity and duration of the disease depend on an individual's health status. Symptoms include diarrhoea and vomiting, nausea, stomach/abdominal cramps, chills, headache, myalgia or malaise. The incubation period ranges from less than 1 day to 4 days. Sapoviruses shedding in faeces may continue after symptoms disappear.
Sapovirus gastroenteritis occurs throughout the year in people of all ages, while sporadic cases occur mainly in the cold seasons. In addition, sapovirus cases appear to be more frequent in younger children than in older children and adults. On the other hand, sapovirus-related gastroenteritis outbreaks have been reported in various settings such as child care centres, kindergartens, nursing homes and schools, where susceptible individuals gathered and where person-to-person transmission was likely involved.
Sapoviruses in Foods
Sapoviruses may be present in shellfish or water environment, as a result of human faecal discharge to the environment. Oysters and clams as well as river water and wastewater have been detected with sapoviruses which are genetically indistinguishable from those clinical isolates. It is believed that sapoviruses can be spread by contaminated shellfish in a way similar to noroviruses. Hence, the preventive measures for noroviruses are also applicable to sapoviruses.
Since oysters feed by filtering a large amount of water through their gills, they are susceptible to contamination if grown in contaminated water. To reduce the risk of contracting sapoviruses, oysters and other bivalves should be cooked thoroughly, i.e. to an internal temperature of 90°C for 90 seconds. Here are some suggestions for cooking time for various preparation methods:
- Boil for 3-5 minutes at 100°C
- Fry for at least 3 minutes at 190°C
- Steam for 4-9 minutes at 100°C
- Bake for at least 10 minutes at 230°C
Susceptible populations (the elderly, young children, pregnant women and people with weakened immune systems) should avoid taking raw oysters.
Food handlers can also be the source of contamination, so personal hygiene is important. They should wash their hands thoroughly with clean running water and soap for 20 seconds after using the toilet and before handling food. Moreover, food handlers with symptoms of vomiting or diarrhoea should not handle food until they are symptom-free for at least two days, and should seek medical advice.
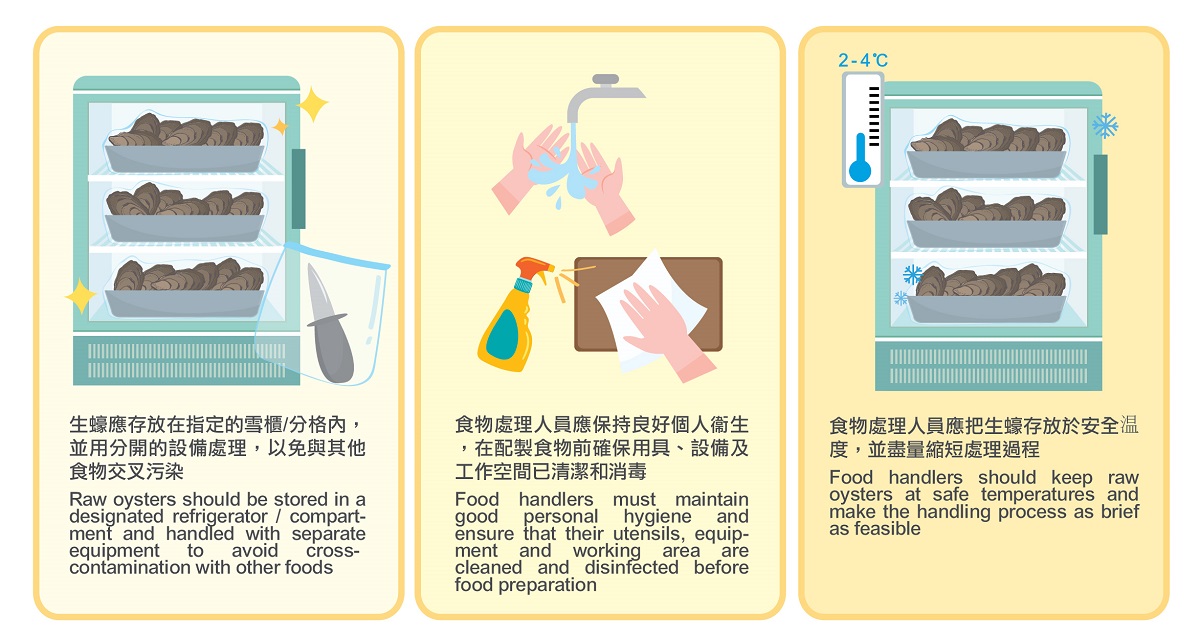
Figure 2: Raw oysters are at high risk for contamination with pathogens and food handlers should adopt relevant food safety measures.

