
Food Safety Focus (172nd Issue, November 2020) – Food Safety Platform
Antimicrobial Resistant Microorganisms – A Food Safety Threat to be Monitored
Reported by Mr. Kenneth YUNG, Scientific Officer,
Risk Management Section, Centre for Food Safety
Antimicrobial resistance (AMR) occurs when microorganisms, commonly bacteria, do not respond to antimicrobial drugs the same way as before. Medicines are therefore less effective against infections caused by AMR microorganisms, otherwise known as 'superbugs'. As a result, infections are more difficult to treat and risks of disease spread, severe illness and death increase. Superbugs are found not only in clinical settings, but also in the environment, animals and food. The situation of AMR has been exacerbated due to factors like misuse of antimicrobials in humans, livestock and agriculture. A comprehensive surveillance programme of AMR collects data under different sectors, which is an integral part of the risk analysis framework from the perspective of food safety. This article aims to discuss the surveillance of AMR in food.
Purpose of Foodborne AMR Surveillance
Surveillance data of foodborne AMR, together with data of antimicrobial use, may help to identify potential relationship between the prevalence of foodborne AMR and the use of antimicrobials in animal sector. Surveillance programme is also one of the sources of information for foodborne AMR risk assessment. It may help authorities to monitor the risk along the food chain, identify new trends of AMR in food, deduce relevant interventions and evaluate their effectiveness.
Surveillance of Foodborne AMR
In view of global concern of the issue, surveillance of foodborne AMR is in place in many parts of the world, e.g. Denmark, the Netherlands and the United States. While the details of foodborne AMR surveillance programmes vary among countries, the World Health Organization and the Food and Agriculture Organization of the United Nations have prepared guidance document or guidelines to assist countries and stakeholders in the development of integrated surveillance programmes of foodborne AMR bacteria.
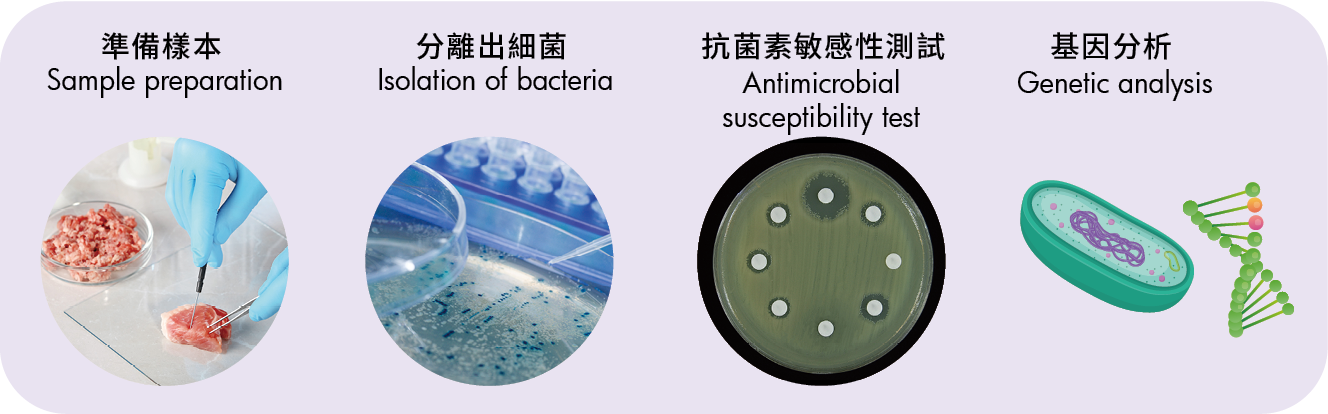
Figure 2: Food samples are prepared and processed so that bacteria present in food can be cultured, isolated and identified. Antimicrobial susceptibility tests are conducted to determine whether the isolated bacteria are susceptible or resistant to certain antimicrobials. Genetic properties of the bacteria are characterised and analysed to better understand the resistance mechanisms.
Type and source of food samples
Various food items, harvested from land or sea, animal or plant origin, raw or ready-to-eat, imported or locally-produced, could be collected for surveillance of foodborne AMR. When deciding the type and source of food samples collected for surveillance, purchasing habits of the consumer, consumption pattern and likely prevalence of AMR in food should be taken into consideration. Food originated from livestock, such as beef, chicken and pork, represents the major route of human exposure to foodborne AMR pathogens, and is therefore the main focus of many surveillance programmes. Other food items such as food of plant origin (e.g. leafy greens) and ready-to-eat food (e.g. sashimi) could also be sampled. Food collected at retail level could facilitate monitoring of foodborne AMR near the end of the food chain.
Type of bacteria to be monitored
Bacteria, such as Escherichia coli and Enterococci, are commonly found in food animals. These bacteria may harbour and transfer resistance genes to human pathogens or other commensal bacteria in the intestine of food animals. Zoonotic bacteria, such as Salmonella and Campylobacter, are also commonly targeted bacteria in many surveillance programmes.
Type of tests and analysis to be conducted
AMR microorganisms are isolated from food samples and then identified. Genetic analysis and typing of bacteria are often conducted to facilitate the characterisation of resistant genes for tracing and epidemiological purposes. Bacterial isolates resistant to three or more classes of antimicrobials are sometimes described as multidrug-resistant, and usually of a higher concern.
Data reporting
Data and results of foodborne AMR surveillance should be communicated with different sectors and stakeholders, with an aim to achieve integration and share of data across sectors with combined reporting of AMR and antimicrobial use, so as to facilitate possible interventions.


